The following is a summary of some recent studies on COVID-19. They include research that warrants further study to corroborate the findings and that has yet to be certified by peer review.
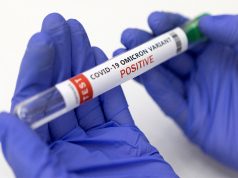
Blood thickness linked with death risk in severe COVID-19
Patients hospitalized with COVID-19 whose blood flows less freely than normal are at higher risk of death from complications, a U.S. study showed. The findings indicate that measurement of blood viscosity, or blood thickness, should be a regular part of these patients’ medical work-up, the researchers said.
High blood viscosity impairs flow to small vessels and increases the risk of blood clots, the researchers noted in the study published on Monday in the Journal of the American College of Cardiology.
Data on 5,621 COVID-19 patients treated at six New York City-area hospitals between February 2020 and November 2021 showed that patients with high viscosity had death rates 38% to 60% higher than those with low blood viscosity.
The inflammation associated with COVID-19 likely contributes to high viscosity, which in turn can lead to damage to blood vessel linings and clogging of arteries, according to the researchers.
“This study demonstrates the importance of checking for blood viscosity in COVID-19 patients early in hospital admission, which is easily obtained through routine lab work,” Dr. Robert Rosenson of the Mount Sinai Health System said in a statement. His team called for further studies to see whether measures to reduce blood viscosity, such as treatment with blood thinning drugs, would be helpful.
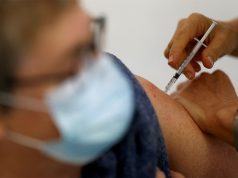
Few excess effects of COVID-19 booster, flu shot together
People who get a flu shot at the same time as a COVID-19 mRNA vaccine booster are only slightly more likely to report side effects than people who get the booster by itself, U.S. researchers found. Earlier studies found that giving flu shots and COVID-19 vaccines at the same time did not make either one less effective and may be more convenient.
As reported on Friday in the journal JAMA Network Open, researchers tracked 981,099 American teens and adults who got vaccine boosters with or without flu shots in September or October 2021.
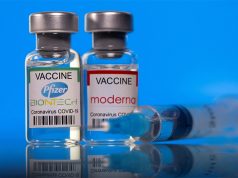
In the following week, reports by study participants of a “systemic” reaction such as fatigue, headache or body aches were 8% higher for those who simultaneously received the flu shot and the Pfizer-BioNTech booster and 11% higher for those who got the flu shot and a Moderna booster, compared to the risk in people who received only an mRNA vaccine booster.
Based on the results, “clinicians can confidently inform patients that concurrent administration of the COVID-19 booster and seasonal influenza vaccine is both safe and associated with only a slight increase in adverse events compared with the COVID-19 booster alone,” a separate team of researchers wrote in an accompanying editorial.
Kids with vaccine allergies safely receive Pfizer shots
The Pfizer mRNA COVID-19 vaccine can be safely given to children even after a suspected allergic reaction to the first dose or a suspected allergy to vaccine ingredients polyethylene glycol (PEG) or polysorbate, according to immunologists. Other allergists previously reported that second doses can be given to adults with suspected reactions to the first dose.
Study results involving a small number of children were published on Wednesday in The Journal of Allergy and Clinical Immunology: In Practice.
At a specialized vaccine clinic, nine children were evaluated after having an allergic reaction to the first dose of the vaccine, including three who experienced potentially life-threatening anaphylaxis.
All nine children – including one who was premedicated – eventually received the second dose “with minimal or no symptoms,” the researchers said. Another three children with histories of potential PEG/polysorbate reactions opted to receive the vaccine at the clinic and tolerated both doses without allergic symptoms.
“Any child who experiences potential anaphylaxis following vaccination should absolutely be evaluated,” study leader Dr. Joel Brooks of Children’s National Hospital in Washington said in a news release.
“The benefits and risks must be weighed carefully when it comes to a second dose. However, we have demonstrated that for this study, most of the initial allergic reactions did not meet the criteria of anaphylaxis and our participants were able to tolerate a second dose of the vaccine.”
—Reporting by Nancy Lapid; Editing by Will Dunham