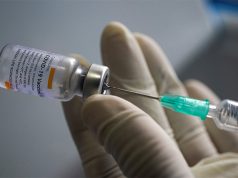
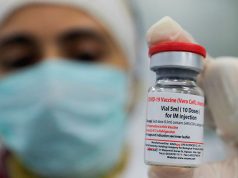
Doctors disproved misconceptions about COVID-19 vaccines amid the proliferation of online rumors that discourage the public from getting inoculated.
With the expected arrival of COVID-19 vaccine this month, the fear of vaccination still runs high among Filipinos online due to trust issues with the country’s health system and other misleading information online.
So far, the vaccines developed by Pfizer-BioNTech, which boasts a 95% efficacy rate, and by Oxford-AstraZeneca, which has 70% efficacy rate on average, are the ones approved for emergency use by the country’s Food and Drug Administration.
How do COVID-19 vaccines work?
In the position statements of the Philippine Society of Allergy, Asthma, and Immunology (PAAI) on COVID-19 Vaccines and their Adverse Reactions released on February 1, the organization explained that the vaccines under trial tests basically use the same “spike protein” of the SARS CoV-2 to kill the cells infected with the virus.
With the same protein, they will stimulate the body’s immune system and prepare the immune cells (T helper cells, B cells, cytotoxic cells) should the person get infected.
“Once natural infection occurs and the virus enters the body, the patrolling immune cells and the specific neutralizing antibodies will recognize the spike proteins and prevent the virus from entering and infecting the host’s cells,” the position statement reads.
“It also starts a cascade of events that leads to activation, proliferation, and enhancement of function of many types of immune cells which results to a stronger response,” it added.
There are four different ways or platforms that the vaccines can stimulate the immune system, namely, the messenger RNA (mRNA), the viral vectors, the protein subunit and the inactivated virus.
Here are the available vaccines under each type:
The messenger RNA (mRNA)
- Pfizer-BioNTech (BNT162b2/Tozinameran/Comirnaty)
- Moderna COVID-19 vaccine (mRNA-1273)
The viral vector
- Oxford-AstraZeneca (ChAdOx1 nCoV-19) – chimpanzee AdV
- Gamaleya Research Institute (Gam-COVID-Vac) – Ad5/Ad26
Protein subunit
- Novavax (Phase III)
Whole inactivated virus
- Sinovac (Coronavac)
- Sinopharm
Clarifying COVID-19 misconceptions
On altering the person’s DNA
In a tweet, physician-scientist Melvin Sanicas stressed that COVID-19 vaccines, particularly the mRNA vaccines, can neither alter nor interact with a person’s DNA.
“COVID-19 vaccines DO NOT alter / interact with your DNA. mRNA does not enter the nucleus, which houses DNA. It works in the cytoplasm, the fluid within a cell. mRNA DOES NOT stick around either. It dissolves once it’s sent a message to cells and exits the body,” Sanicas said.
The Pfizer-BioNTech, which falls under the mRNA type, is one of the most preferred brands by Filipinos due to its reported high efficacy rate.
Last January 14, the John Hopkins Bloomberg School of Public Health also released a video on how the mRNA vaccine works.
Allergies are rare but may occur
Rheumatologist Geraldine Zamora cited a presentation by Dr. Regina Berba, chairperson of the Hospital Infection Control Unit-Philippine General Hospital, who emphasized the possibility of allergic reactions.
Allergy is rare but may occur.
Therefore IT IS IMPORTANT that the facility is able to address the potential reactions. The hospitals will observe vaccinees for 30 to 60minutes.
– Dr. Regina Berba<Huwag po basta basta magpabakuna kung saan saan kung hindi kayo mababantayan.> pic.twitter.com/p0Klq7mTpd
— Dr. Geraldine Zamora (@doktora_ging) February 8, 2021
Berba was quoted as saying that patients who are vaccinated should be observed or monitored in hospitals between 30 to 60 minutes.
In the screenshot of the slide Zamora attached, it was stated that patients who have immediate allergic reactions whether it be mild (rashes) or severe (anaphylaxis) after the first dose should not receive another.
“Huwag po basta basta magpabakuna kung saan saan kung hindi kayo mababantayan,” Zamora said in a Twitter thread.
Zamora also noted that those with food allergies should seek assistance from their allergists first.
On contraindication to vaccines
In line with allergies, the PAAI in its position statements said that patients who should not be given a COVID-19 vaccine are those who have allergic reactions to certain vaccine substances called excipients.
These excipients are:
- Polyethylene glycol (PEG) – found in colonoscopy preparation, or laxatives; PEG 2000 is found in mRNA vaccines.
- Polysorbate – found in vascular graft materials, surgical gels, PEGylated medications; Polysorbate 80 can be found in non-replicating adenovirus vector vaccines and protein subunit vaccines.
“Patients who have experienced an immediate allergic reaction, such as urticaria, angioedema, difficulty of breathing, regardless of severity, to any OTHER vaccine or injected therapy must be evaluated by an allergist to assess possible allergic reactions to PEG or polysorbate,” PAAI said.